Staff Perspective: The Virtual Hope Box!
Electronic Health (eHealth) has long been integrated into the mental health field allowing for healthcare practices supported by electronic processes or communication. One type of eHealth is Mobile Health (or mHealth) interventions, which refers to the use of mobile devices for a number of activities that could include Internet access or searches, text messaging as well as smart phone applications that could be used within a mental health context. Although research remains limited, attention to mobile apps has been rapidly growing due to the increased use of technology in the mental health field. Mobile mental health support can be very simple but effective, providing users with convenience, anonymity, consistency and round-the-clock service. Often, technology is utilized to complement traditional therapy rather than replace it.
The Virtual Hope Box (VHB) was developed by Nigel Bush, a research psychologist for the Defense Department’s National Center for Telehealth & Technology (T2), a component center of the Defense Centers of Excellence for Psychological Health and Traumatic Brain Injury. It is available as a free download on iOS and Android platforms. The Virtual Hope Box (VHB) is a smartphone tool for moments of crisis and is intended to supplements treatments already happening. The purpose of the VHB is to help patients decrease subjective experience of distress by facilitating adaptive coping and emotion regulation skills. The VHB was awarded the 2014 Department of Defense Innovation Award, as a result of the unique way that it has applied technology in supporting behavioral health for Service members and their families. To download the VHB on your device, log on to the Apple App Store or Android Market.
Hopelessness is one of the greatest risk factor for suicide. Accordingly, one way to challenge suicidal ideations and urges is to cultivate hope. One key intervention that mental health specialists have traditionally used to cultivate hope is to create a “Hope Box”—a collection of various items that remind the patients that their lives are meaningful and worth living. A Hope Box can include anything from photos of loved ones, letters, special tokens or certificates of past achievements, inspirational quotes, a list of future aspirations, CDs of relaxing music, and religious verses, to coping skills and tools developed during treatments (e.g., coping cards, a copy of one’s Safety Plan, distraction techniques etc.). In reality, a Hope Box can include anything that reminds the individual of reasons to stay alive and/or helps to provide distraction from suicidal thoughts.
The rationale behind the Hope Box is straightforward; individuals who are acutely distressed may, at times, struggle to recall all the positive aspects of their life. This occurs as a result of a process termed cognitive constriction, which prevents individuals in overwhelming pain from perceiving ways to end their emotional pain in ways other than suicide. A Hope Box is a powerful strategy to help those considering suicide access tangible reminders of reasons for living. Placing everything in one accessible spot can help to eliminate the problem of cognitive constriction. By creating the Hope Box in advance, the individual is able to arm himself/herself against the tunnel vision and distorted thinking that will likely occur when experiencing suicidal thoughts.
The Hope Box itself can take various forms: a real wooden box or shoe box, a manila envelope, a plastic bag, or anything else. Although the Hope Box is a key therapeutic component in common treatments targeting suicidal ideation and behaviors, it can be physically cumbersome and inconvenient; more importantly it is often not available when a patient needs it most during crises. Service members and Veterans might find it inconvenient to take the Hope Box to work or might find it inconvenient to carry it when traveling. To overcome this barrier, Nigel Bush and his colleagues at the National Center for Telehealth and Technology have designed a “Virtual Hope Box,” a smartphone app that allows the patient to keep their Hope Box wherever they go. Because mobile devices such as smartphones are carried all the time, they can expand the reach of traditional therapeutic interventions. Not only is this more convenient for Service members who are highly mobile, but it can be available during suicidal crises, which often emerge in the absence of healthcare providers.
Here is a screen shot of the main Virtual Hope Box screen and the features it offers.
The app includes the following features:
- Key Contacts: This feature provides users with information on how to access support through various means, including crisis resource information (e.g., 911, the Veterans Crisis Line and the DCoE Outreach Center). In addition, it provides users with the option of incorporating key contacts and their individualized support network, including people who have agreed to be available for a phone call in a time of crisis.
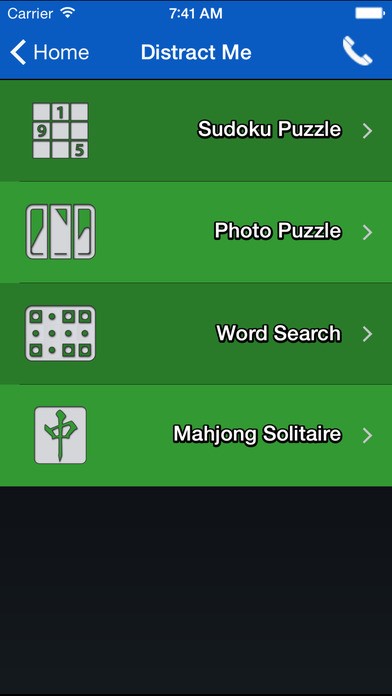
- Distract Me: This section includes an activity planner and puzzles/word search games taken from user content.
- Inspire Me: This section provides users with preloaded inspirational quotes, which can be supplemented or replaced by personal quotes, family aphorisms, biblical phrases, etc. Users can set a daily reminder to receive daily inspirational quotes if desired.
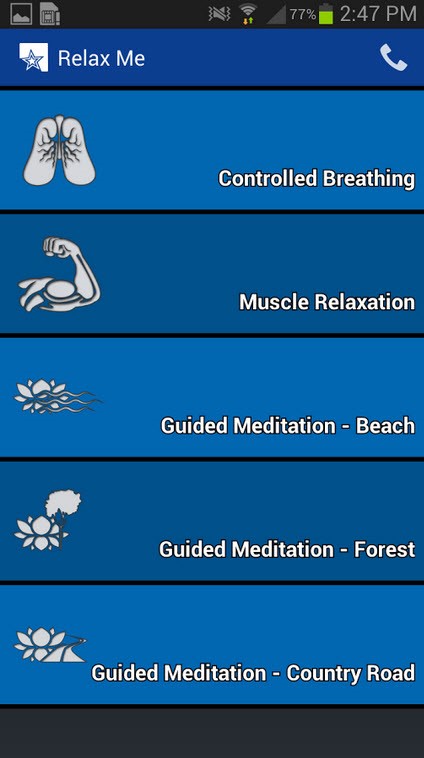
- Relax Me: This section provides users with relaxation exercises to help them calm down, including a deep breathing tool, progressive muscle relaxation, etc.
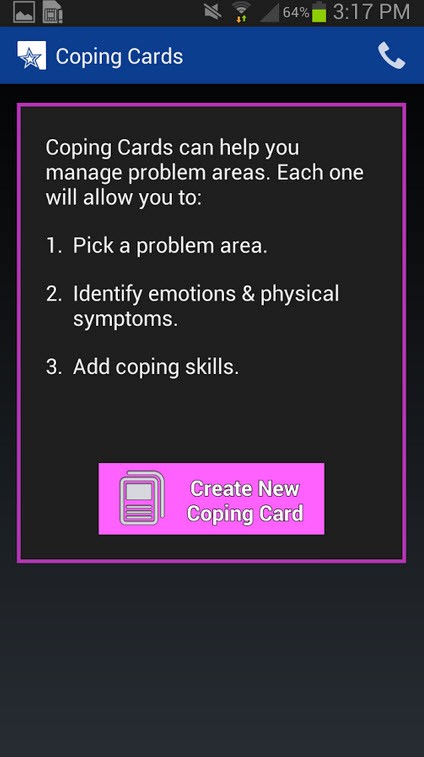
- Coping Tools: This section provides a collection of “coping cards” in which the patient has written down positive, realistic and adaptive thoughts and behaviors to use when in crisis or to manage problematic core beliefs. In addition, an Activity Planner is incorporated allowing users to schedule and track their activities, as well as invite others to participate in activities, thereby enhancing their social support network.
- Disclaimer: While the Virtual Hope Box can be a helpful tool to augment psychotherapy or cultivate hope, it is not intended to replace psychotherapy for those who need it.
For more information on other apps that providers may find useful, please visit the “Apps” section of CDP’s website here. You can also check out the CDP Presents webinar "Use of Mobile Applications in Clinical Practice" or check out Dr. Jenna Ermold’s “Got Apps?” or Dr. Marjorie Weinstock’s “Behavioral Activation - There’s an App for That!”. Feel free to share any useful apps you’ve found in the comments below or send us an email and we’ll try to feature them on the blog!
The opinions in CDP Staff Perspective blogs are solely those of the author and do not necessarily reflect the opinion of the Uniformed Services University of the Health Science or the Department of Defense.
References:
Bush, N., Kinn, J., Higgins, M., Turney-Loos, W., Hoffman, J., Dobscha, S., & Denneson, L. (2014). Development and Evaluation of a Virtual Hope Box for Reducing Suicidal Ideation.
Jobes, D.A. (2006). Managing suicidal risk: A collaborative approach. New York, NY: The Guilford Press.
Sharon Birman, Psy.D., is a CBT trainer working with the Military Training Programs at the Center for Deployment Psychology (CDP) at the Uniformed Services University of the Health Sciences in Bethesda, Maryland.
Electronic Health (eHealth) has long been integrated into the mental health field allowing for healthcare practices supported by electronic processes or communication. One type of eHealth is Mobile Health (or mHealth) interventions, which refers to the use of mobile devices for a number of activities that could include Internet access or searches, text messaging as well as smart phone applications that could be used within a mental health context. Although research remains limited, attention to mobile apps has been rapidly growing due to the increased use of technology in the mental health field. Mobile mental health support can be very simple but effective, providing users with convenience, anonymity, consistency and round-the-clock service. Often, technology is utilized to complement traditional therapy rather than replace it.
The Virtual Hope Box (VHB) was developed by Nigel Bush, a research psychologist for the Defense Department’s National Center for Telehealth & Technology (T2), a component center of the Defense Centers of Excellence for Psychological Health and Traumatic Brain Injury. It is available as a free download on iOS and Android platforms. The Virtual Hope Box (VHB) is a smartphone tool for moments of crisis and is intended to supplements treatments already happening. The purpose of the VHB is to help patients decrease subjective experience of distress by facilitating adaptive coping and emotion regulation skills. The VHB was awarded the 2014 Department of Defense Innovation Award, as a result of the unique way that it has applied technology in supporting behavioral health for Service members and their families. To download the VHB on your device, log on to the Apple App Store or Android Market.
Hopelessness is one of the greatest risk factor for suicide. Accordingly, one way to challenge suicidal ideations and urges is to cultivate hope. One key intervention that mental health specialists have traditionally used to cultivate hope is to create a “Hope Box”—a collection of various items that remind the patients that their lives are meaningful and worth living. A Hope Box can include anything from photos of loved ones, letters, special tokens or certificates of past achievements, inspirational quotes, a list of future aspirations, CDs of relaxing music, and religious verses, to coping skills and tools developed during treatments (e.g., coping cards, a copy of one’s Safety Plan, distraction techniques etc.). In reality, a Hope Box can include anything that reminds the individual of reasons to stay alive and/or helps to provide distraction from suicidal thoughts.
The rationale behind the Hope Box is straightforward; individuals who are acutely distressed may, at times, struggle to recall all the positive aspects of their life. This occurs as a result of a process termed cognitive constriction, which prevents individuals in overwhelming pain from perceiving ways to end their emotional pain in ways other than suicide. A Hope Box is a powerful strategy to help those considering suicide access tangible reminders of reasons for living. Placing everything in one accessible spot can help to eliminate the problem of cognitive constriction. By creating the Hope Box in advance, the individual is able to arm himself/herself against the tunnel vision and distorted thinking that will likely occur when experiencing suicidal thoughts.
The Hope Box itself can take various forms: a real wooden box or shoe box, a manila envelope, a plastic bag, or anything else. Although the Hope Box is a key therapeutic component in common treatments targeting suicidal ideation and behaviors, it can be physically cumbersome and inconvenient; more importantly it is often not available when a patient needs it most during crises. Service members and Veterans might find it inconvenient to take the Hope Box to work or might find it inconvenient to carry it when traveling. To overcome this barrier, Nigel Bush and his colleagues at the National Center for Telehealth and Technology have designed a “Virtual Hope Box,” a smartphone app that allows the patient to keep their Hope Box wherever they go. Because mobile devices such as smartphones are carried all the time, they can expand the reach of traditional therapeutic interventions. Not only is this more convenient for Service members who are highly mobile, but it can be available during suicidal crises, which often emerge in the absence of healthcare providers.
Here is a screen shot of the main Virtual Hope Box screen and the features it offers.
The app includes the following features:
- Key Contacts: This feature provides users with information on how to access support through various means, including crisis resource information (e.g., 911, the Veterans Crisis Line and the DCoE Outreach Center). In addition, it provides users with the option of incorporating key contacts and their individualized support network, including people who have agreed to be available for a phone call in a time of crisis.
- Distract Me: This section includes an activity planner and puzzles/word search games taken from user content.
- Inspire Me: This section provides users with preloaded inspirational quotes, which can be supplemented or replaced by personal quotes, family aphorisms, biblical phrases, etc. Users can set a daily reminder to receive daily inspirational quotes if desired.
- Relax Me: This section provides users with relaxation exercises to help them calm down, including a deep breathing tool, progressive muscle relaxation, etc.
- Coping Tools: This section provides a collection of “coping cards” in which the patient has written down positive, realistic and adaptive thoughts and behaviors to use when in crisis or to manage problematic core beliefs. In addition, an Activity Planner is incorporated allowing users to schedule and track their activities, as well as invite others to participate in activities, thereby enhancing their social support network.
- Disclaimer: While the Virtual Hope Box can be a helpful tool to augment psychotherapy or cultivate hope, it is not intended to replace psychotherapy for those who need it.
For more information on other apps that providers may find useful, please visit the “Apps” section of CDP’s website here. You can also check out the CDP Presents webinar "Use of Mobile Applications in Clinical Practice" or check out Dr. Jenna Ermold’s “Got Apps?” or Dr. Marjorie Weinstock’s “Behavioral Activation - There’s an App for That!”. Feel free to share any useful apps you’ve found in the comments below or send us an email and we’ll try to feature them on the blog!
The opinions in CDP Staff Perspective blogs are solely those of the author and do not necessarily reflect the opinion of the Uniformed Services University of the Health Science or the Department of Defense.
References:
Bush, N., Kinn, J., Higgins, M., Turney-Loos, W., Hoffman, J., Dobscha, S., & Denneson, L. (2014). Development and Evaluation of a Virtual Hope Box for Reducing Suicidal Ideation.
Jobes, D.A. (2006). Managing suicidal risk: A collaborative approach. New York, NY: The Guilford Press.
Sharon Birman, Psy.D., is a CBT trainer working with the Military Training Programs at the Center for Deployment Psychology (CDP) at the Uniformed Services University of the Health Sciences in Bethesda, Maryland.